Making sure a patient completely understands the details about their upcoming procedure is crucial to truly informed consent. For two decades EIDO Healthcare have been supplying health professionals with resources and support to aid the consent process and make the conversations around it more harmonious for both doctor and patient.
Consent is the voluntary and continuing permission of a patient with capacity to receive a particular treatment, based on an adequate knowledge of the purpose, nature and likely risks of the treatment, including the likelihood of its success and any alternatives to it. Permission given under any unfair or undue pressure is not consent.
Code of Practice: Mental Health Act 1983 (1)
Challenge – Staying up to date
The law surrounding consent is continually changing and keeping up to date with these changes poses a challenge to clinicians. With very little free time, health professionals need a way of keeping on top of many of the changes to consent law without it consuming too much time.

EIDO’s solution
For the last three years, we’ve released our free Consent Reviews. These reviews examine notable court cases in the wake of the landmark Supreme Court ruling in the case of Montgomery in 2015 and draws out crucial guidance and lessons for clinicians to help them navigate the turbulent era of informed consent.
The author, Vivienne Harpwood, is Emerita Professor of Healthcare Law at Cardiff University, Chair of Powys Health Board and Chair of the Welsh NHS Confederation. Her many years’ experience within this area provides an invaluable insight into the world of consent law. Vivienne is currently working on the fourth edition of our Consent Review, which will be released later this year. To download a free copy of the third edition, please visit the EIDO Healthcare Website.
Consent law is a highly complex area, and one that is constantly evolving as new cases are decided by the courts. Never before has it been so important for clinicians to have a proper understanding of their responsibilities, and to obtain consent to treatment within the boundaries set by the law.
Simon Parsons, Divisional Director of Surgery at Nottingham University Hospitals NHS Trust, Technical Director at EIDO Healthcare (2)
Challenge – Litigation
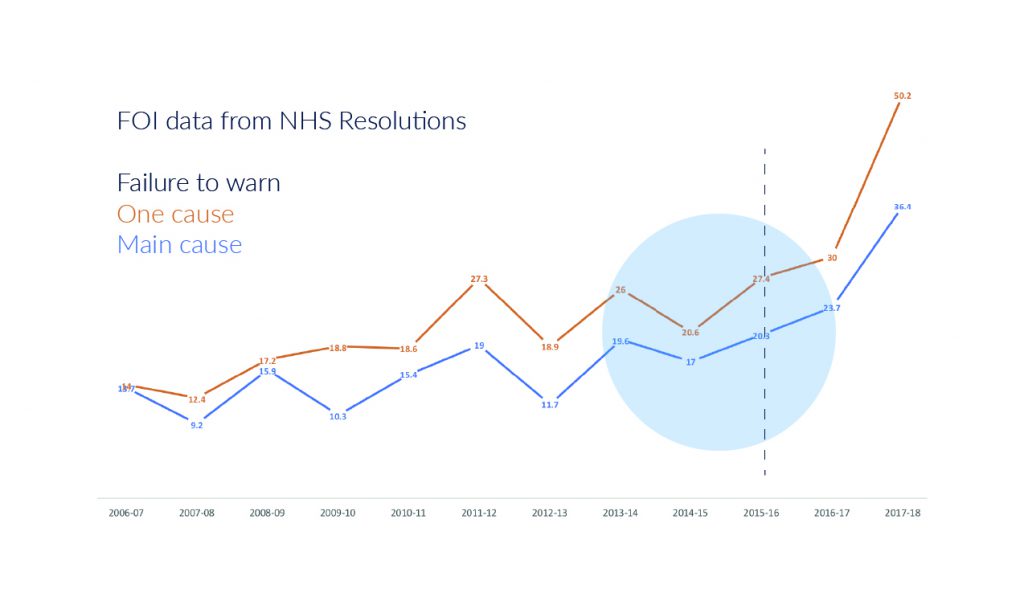
Data obtained by Freedom of Information requests, has found that in ten years, consent-related litigation costs for “failure to warn” have risen by 295%. Risk of litigation is a persistent problem and can arise if the conversations between a doctor and their patient aren’t properly recorded.
The data also indicates that hospitals who licenced our library paid out, on average, 25% less in litigation fees than hospitals using other sources of information.
EIDO’s solution
In order to avoid accusations of litigation, there needs to be a better way of keeping track of the information patients receive and clear signs that they have understood it. Our products were created to establish better and more robust ways of obtaining and recording consent. Our new product Inform Digital allows patients to read EIDO documents using a smartphone, tablet or computer from the comfort of their own home, where they can concentrate and better absorb the information. It also tracks patient engagement, recording how long the patient spends reading the information to measure how much they engaged with it.
Challenge – Keeping information current
Medical procedure methods are constantly being reviewed and improved. As new research comes to light, risk rates and best practice changes. Information documents given to patients must be current and amendments to laws and guidance around best practice must be reflected in them quickly.
EIDO’s solution

All of our documents are up to date and in line with best medical practice. We ensure this through regular reviews to our library and a publishing system which delivers speedy updates. Any changes we make to our documents are visible the very next day and our customers are then notified about changes via our download centre homepage.
Our content is also reviewed for readability by the Plain English Campaign. Every document in our Inform library receives the Plain English Campaign ‘Crystal Mark’, their seal of approval that our documents are well-written and easy to read.
You must work in partnership with your patients. You should discuss with them their condition and treatment options in a way they can understand, and respect their right to make decisions about their care.
General Medical Council (3)
Why not get in touch today to see how we can assist you with any challenges you face around informed consent?
To chat over the phone, call us on +44 115 878 1000
Or to send us an email at [email protected]
(1) ‘Code of Practice: Mental Health Act 1983’, Department of Health (2015), p. 257 (https://assets.publishing.service.gov.uk/government/uploads/system/uploads/attachment_data/file/435512/MHA_Code_of_Practice.PDF).
(2) Consent Review: Second Edition, EIDO Healthcare (2018), p. 1.
(3) ‘Consent: patients and doctors making decisions together’, General Medical Council (2014), p. 5 (https://www.bahrs.co.uk/content/large/documents/patient_advice/rcs_consent_ntwc05-app1-conspts-drsmakingdecisions-v04-issjan16.pdf).











